[6 MIN READ]
[6 MIN READ]
The national nursing shortage makes recruiting and retaining quality nursing staff extremely competitive. While facilities traditionally might have required 3-5 years of emergency department (ED) experience before training a nurse for triage, the lack of resources has forced some organizations into reducing the requirement to one year or less. As this requirement decreases, it is increasingly critical to have a well-defined onboarding path for nurses new to triage.
Additionally, having well-defined role expectations – especially during onboarding – can have a significant impact on a nurse’s job satisfaction and the likelihood they will stay with your organization.
The Focus of Onboarding
While new nursing graduates have the formal nursing training necessary to become RNs, they generally lack the knowledge and critical thinking skills that are developed only after years of practicing in the ED trenches caring for agitated patients, managing overcrowded waiting rooms, and experiencing missed diagnoses firsthand.
Since the goal of triage is the rapid and accurate assignment of a triage acuity level (link to blog), your onboarding process should focus on:
- Closing the knowledge gaps
- Recognizing red flags of demise
- Exposing new hires to real patient scenarios
- Avoiding the common pitfalls of high-risk presentations
- Educating on general risk management and patient safety
This checklist was created to provide you with a template to not only provide the right training for your new hires, but also a framework through which you can validate their triage competency.
1) Determine What to Train
Once you have selected candidates who have the potential to be successful triage nurses, it is critical to establish a baseline level of triage competency. While considering the goals of your program, you should define in writing what this means for your organization:
- What’s required to do their job in the first 6 months?
- What high-risk accountabilities will the nurse be engaged in?
- What core job functions do you expect when you initially hire them?
As a standard, all triage nurses must have a concrete understanding of the following concepts before being released to triage independently:
- Risks related to triage, including malpractice, reassessment and documentation
- Triage practice standards, including ESI, CTAS, and collection and reassessment requirements outlined by regulatory bodies like The Joint Commission, the Emergency Nurses Association (ENA), and your own organization
- Triage assessment and documentation, including systems, chief complaints, risk factor analysis, vital signs, and pain assessment
- Triage policy, procedures and guidelines, including evidence-based practice, EMTALA, and frequency of competency validation
Position the weight and importance of triage competence by communicating the following from ENA’s Scope and Standards of Practice (2011):
“The Emergency RN triages each healthcare consumer utilizing age, adjusting to be developmentally appropriate, and using culturally sensitive practices to prioritize and optimize healthcare consumer flow, expediting those healthcare consumers who require immediate care.”
“Rapid, efficient triage and judicious care contribute to optimal healthcare consumer outcomes.”
2) Define Training Structure
Once you have defined the baseline competencies for a triage nurse, your program should then outline how a new triage nurse will be trained and tested on these concepts.
A new hire should expect to successfully complete the following before being released to triage independently:
- Probationary period
- General ED orientation
- Formal triage education program
- Six-month performance assessment/evaluation
- Period for triage observation with a preceptor
- Any additional requirements laid out by your health system
3) Create Triage Education Program
The goal of a triage education program should be to fill the knowledge gaps commonly seen between a new hire and an experienced triage nurse. Each new hire should successfully compete a formal education program.
If the new hire has prior healthcare experience, an organization might modify their formal education requirements or timeline. Some organizations offer a test-out option for experienced new hires to bypass certain courses.
An example of a best practice online education program is The Sullivan Group's Triage Fundamentals Program (link to sales page), created by experienced triage trainers, to ensure nurses have a concrete understanding of the core concepts critical to triage success. You can read more about how to structure a triage education program here.
As you evaluate triage training programs, be mindful that each nurse has a unique learning style. You might complement an online learning program with live education seminars and self-study materials.
Make sure your program incorporates adult learning best practices to give new hires the best opportunity to retain concepts. As a model, The Sullivan Group’s education programs are built upon these five RSQ® Education Pillars for educational excellence. Learn more by watching this video outlining our pillars of educational excellence.
4) Teach the Domains of Triage Competency
Make sure staff understand what constitutes triage competence. Communicate that they will be assessed on the 3 Domains of Competency, as defined by Donna Wright (link) and applied to Triage:
- Technical
- Does the nurse assign the correct triage levels?
- Does the nurse follow standing orders/protocols?
- Is documentation accurate and complete?
- Critical Thinking
- Does the nurse rapidly identify common red flags?
- Does the nurse apply lessons from previous events?
- Does the nurse connect risk factors to presentation?
- Interpersonal
- Does the nurse effectively communicate with team leader/charge nurse?
- Does the nurse demonstrate respect for a diverse patient population?
- Does the nurse manage angry/aggressive patients safely, efficiently and effectively?
5) Select Triage Competency Validation Methods
It is critical for new hires to understand that knowledge and competence are different. Completing a course instills knowledge – an understanding of the facts; it does not demonstrate their competence – the ability, skill and aptitude to apply that knowledge in a real patient scenario.
There are several methods available to validate triage competency, including:
- Direct observation – performed in real-time, in a simulation experience, or in a computer program
- Case scenario packets – can be done during or after a triage class
- Written assessment – used after a triage class or online learning activity
- Exemplars – can be written or group discussion with a prompt, such as "My greatest triage challenge ... " or "I struggle when ..."
- Staff meeting case presentations – staff listen and discuss
- Retrospective chart review – review of triage record by self or peers
- Self-assessment – retrospective review of triage decisions and interpersonal skills compared to the assessment of a peer or manager
Each of these methods has its strengths and weaknesses. An effective competency validation program uses a variety of these methods and changes out methods every few quarters to both identify additional opportunities for improvement and provide variety for staff.
With these steps in mind, outline your expectations matrix so new hires understand what to expect from their onboarding period. Below is a sample framework that can be used as a starting point to be modified to fit an organization.
|
Year 2020 |
RN |
Experience |
Triage Course |
Chart Reviews |
Validation |
|
Novice Nurse |
X |
6 months |
X |
Self + Preceptor |
|
|
Experienced New Hire |
X |
90-day probation |
Test-out option |
Monthly x 3 |
|
|
Current Staff |
X |
Ongoing |
Bi-annual update |
Quarterly by category |
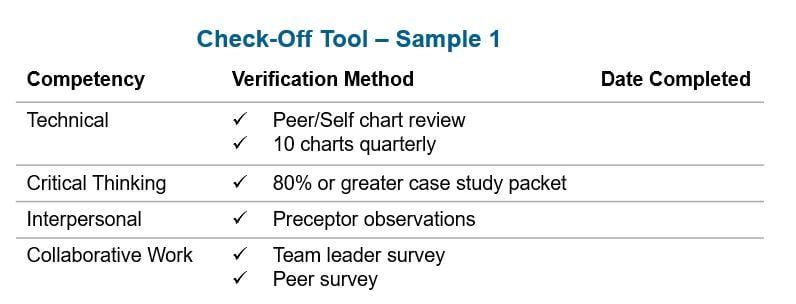

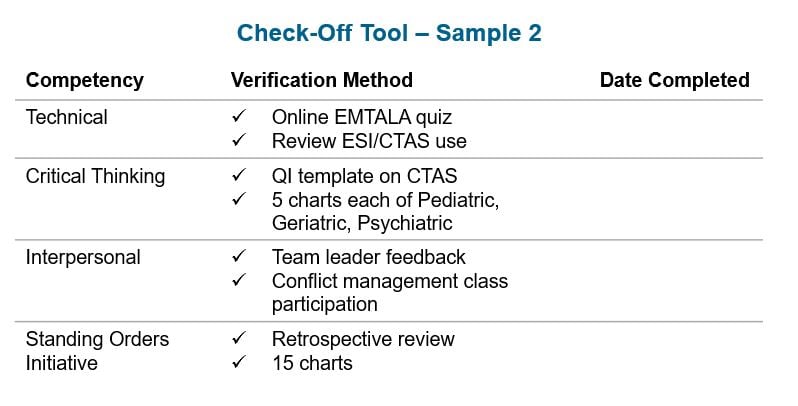
This competency matrix and these check-off tools aid in holding staff accountable while providing a clear outline of what is expected of each nurse.
6) Remediation Options
To promote consistency in triage, it is critical to communicate what happens if a nurse does not meet expectations. Each department should have a written policy describing options available for remediation. The policy should address a variety of situations, including:
- Failure to complete within allotted time frame
- Failure to meet competency standards
- When remediation is appropriate and the acceptable methods (e.g., increased chart review or observation)
- When dismissal from the department is considered in the interest of patient safety
7) Update Regularly
As standards, policies and protocols change, your onboarding process and materials will need to be updated regularly. We recommend reviewing at least once a year to ensure the process remains effective.
8) Transition to Ongoing Competency Validation
The ENA outlines that “triage competency assessment should not be a one-time event, but rather a fluid, dynamic process, with periodic assessment of all nurses who practice this high-risk skill.” (link to the 2017 position statement).
Once a new hire completes your initial triage competency process, they should be transitioned into your ongoing competency validation cycle.
Summary
Nurses stay in roles where they feel valued, respected and appreciated. A well-defined onboarding process to triage provides each new nurse the opportunity to understand what it takes to be successful within their new role and allows them to fulfill their greatest potential within your organization. We hope this checklist guides you toward a system you can feel confident will improve consistency in triage and ensure high-quality patient care.