 [4 MIN READ]
[4 MIN READ]
Every day, ED physicians, physician assistants, nurse practitioners and nurses are confronted with pediatric patients suffering from infections. Thankfully, most are self-limited respiratory or gastrointestinal viral infections.
Symptomatic and supportive care may be necessary, but antibiotics are not usually indicated; minor infections such as otitis media, impetigo, pharyngitis and uncomplicated urinary tract infections usually respond well to either oral antibiotics or a single parenteral dose of an antibiotic.
When treating an infant or a child with an infectious process, it is important to check for and recognize the subtle warning signs and symptoms of a more serious infection – whether viral or bacterial. When overlooked in their earliest stages, several types of infections can progress to life- or limb-threatening situations. Failing to consider and test for the possibility of serious infections in children can lead to serious, even fatal, outcomes.
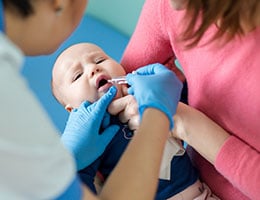
Immunizations for serious diseases caused by Haemophilus influenza Type B (Hib), Pneumococcus, Meningococcus, measles, mumps and pertussis have been successful in greatly reducing the burden of disease and death from these infectious agents.
However, we are now seeing a resurgence of these preventable diseases, primarily due to lack of preventive vaccination and the lack of herd immunity provided by vaccination. Non-immune individuals include populations for whom vaccination is neither affordable nor accessible and those who have chosen not to vaccinate. Putting aside the ethical, moral and personal debates regarding vaccination vs. non-vaccination, here are some highlights of the six aforementioned largely preventable causes of serious childhood infections.
Haemophilus influenzae Type B (Hib)
- It is an invasive bacterial disease that causes meningitis, sepsis, epiglottitis, pneumonia, septic arthritis, osteomyelitis, pericarditis and cellulitis.
- Prior to the Hib vaccine, Hib was the leading cause of bacterial meningitis in the U.S. in children <5 years old, resulting in a 4% fatality rate and complications such as hearing impairment or severe neurologic sequelae in 15% to 30% of those who survived.
- Only the most “seasoned” practitioners will recall ever aspirating a subdural empyema through the fontanelle of an infant with H. flu meningitis.
- Vaccination has reduced the incidence of invasive Hib infections by 99% in children <5 years old.
- Most Haemophilus infections are now caused by types other than Type B.
Pneumococcus
- It is a bacterial infection caused by Streptococcus pneumoniae; there are >90 types.
- It remains a common and leading cause of otitis media, pneumonia, meningitis and bacteremia, causing more than 4 million infections and 22,000 deaths annually.
- Children <2 years and adults >65 are at greatest risk for serious infections.
- Vaccinations have evolved to more effectively cover the most common serotypes responsible for serious infections.
- Antimicrobial resistance has become very common, with inappropriate antibiotic therapy contributing to the development of drug resistant Strep pneumoniae.
Meningococcus
 It is a life-threatening infection caused by 12 serogroups of Neisseria meningitidis bacteria; 6 of these groups cause most cases.
It is a life-threatening infection caused by 12 serogroups of Neisseria meningitidis bacteria; 6 of these groups cause most cases.- Clinical presentation may include sudden onset fever, neck stiffness, nausea, vomiting, confusion, lethargy, and a rash that is petechial or purpuric.
- It progresses to severe illness and death in the absence of immediate treatment.
- Diagnosis is difficult in early stages due to non-specific symptoms and signs.
- It is transmitted person-to-person through direct contact or droplet transmission.
- Incidence is highest in infants <1 year of age.
- Meningitis occurs in 50% of invasive cases; bacteremia is present in 40% of cases of meningococcal infection. Bacteremia presents as fever and rash, and progresses to hypotension, multiple organ failure, shock, and eventually death – often in a very rapid progression.
- Vaccination is recommended for routine use and for those patients with conditions that place them at high risk for meningococcal infection.
Measles
- A highly contagious viral illness, usually mild or moderate, with symptoms of fever, coryza, cough, malaise, conjunctivitis and a maculopapular rash that spreads from head to trunk to legs.
- Can be complicated by encephalitis, pneumonia, and death.
- Pre-vaccine (1963) statistics reveal more than 500,000 cases and nearly 500 deaths reported annually – and there were likely millions more unreported cases.
- Recently, more than 1,200 individual measles cases have been confirmed in 31 states; this is the greatest number of cases reported in the U.S. since 1992.
- Most cases of measles occur in non-vaccinated or under-vaccinated persons.
Mumps
- It is an acute viral illness with a non-specific prodrome of fever, myalgia, anorexia, headache and malaise; it is followed by the classic symptom of parotitis lasting from 2 days to >10 days.
- Prior to vaccine, mumps was very common in deployed military populations.
- Complications include deafness, aseptic meningitis, encephalitis, orchitis and pancreatitis. Permanent neurologic sequelae and death are rare.
- Nearly early 900 confirmed cases have been recently reported by the CDC in adult migrants in 19 states; another 33 cases occurred among staff members.
- Outbreaks of mumps continue to occur despite vaccination and control efforts.
Pertussis
- Known as whooping cough, pertussis is a respiratory disease caused by Bordetella pertussis
- It clinically presents as a paroxysmal cough, often with an inspiratory whoop.
- It rarely produces complications, although infants are at highest risk for complications, including pneumonia, seizures and encephalopathy.
- Prior to vaccines, pertussis was a major cause of infant mortality.
- Incidence has been increasing in recent years since 2012 due to multiple factors, including waning immunity from prior vaccination, improved diagnostic testing, and increased practitioner awareness.
- Incidence is highest among infants <6 months of age.
A key caveat to improving diagnostic accuracy in patients of all ages who present with symptoms and signs of infection is to perform a detailed immunization history.
Due to increased migration of non-vaccinated populations, increased global travel, and a minority of individuals who are non-vaccinated by choice, practitioners who have recently completed training and entered practice will need to become familiar with the epidemiology, clinical presentations, treatment and prevention of these and other serious bacterial and viral infections that were thought to be declining or even eradicated in the U.S. Even seasoned practitioners who encountered these infections “back in the day” will benefit from a review and update.


