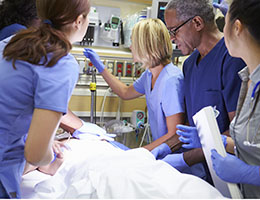
The shortage of nursing professionals is a growing global crisis that significantly impacts patient safety and healthcare delivery systems. Emergency departments (EDs) are particularly impacted, as there are not many nurses still working in EDs who have more than a few years of experience. The importance of an experienced and effective nursing team cannot be overstated both in and outside of the ED. The nursing shortage has a direct impact on patient safety, so this is a good subject for this week’s discussion.