
Because every patient entering the emergency department needs to be triaged, it is imperative to ensure that every triage nurse maintains accurate clinical decision-making skills that support optimization of patient flow. While the Emergency Nurses Association (ENA) has historically recommended ongoing triage competency validation to ensure safe practice in the ED, the organization updated itsTriage Qualifications and Competency Position Statement in 2017 to place greater emphasis on the use of retrospective chart review as a means to ensure accurate clinical decision-making in triage.
In addition to the ENA recommendation, here are five more reasons retrospective chart review is an effective part of a triage competency validation process:
- Reflect on actual patient encounters.
Patients present to the ED with complex chief complaints complicated by co-morbidities, both of which can be difficult enough to navigate before considering if they have any issues accurately communicating their ailments. Because of these hurdles, it’s hard to simulate the wide range of patients a triage nurse may encounter in written cases.
Moreover, written case scenarios might allow for nurses to be overconfident in their abilities; their perception of a quality performance might not match reality. In a study published in the Scandinavian Journal of Trauma, Resuscitation, and Emergency Medicine1, Dr. Jordi wanted to determine the accuracy and inter-rater reliability and subject confidence of triage nurses at four hospitals to determine ESI level. Sixty-nine nurses applied the ESI scale to 30 teaching case scenarios. The study showed these nurses scored only 59.6% of cases correctly, yet 78% of those nurses felt confident in their ability to apply ESI. This study concluded that using written case scenarios to determine ESI scoring accuracy may not be the optimum method to rate a nurse’s triage skills.
When nurses can step outside the hectic environment of the ED, self-evaluated retrospective chart review can allow them to review their own prior cases. They can concentrate on the details of each individual case without interruption to assess whether they might have made any improvements or changes in the evaluation.
- Improve critical thinking skills.
While other methods of triage competency validation serve up case scenarios, a self-evaluated retrospective chart review can allow an individual triage nurse interactive feedback as the patient encounter develops. Using a smart online audit such as RSQ® Solutions - Triage Assessment, triage nurses can be fed critical thinking checkpoints offering feedback as they enter details from their prior patient encounter. These checkpoints can provide valuable insight on areas individual nurses might have missed in their initial assessment and help refine their understanding of the CTAS and ESI classification systems.
For example, a nurse entering details from a chest pain patient encounter might be prompted with critical thinking tips regarding the recommended time within which chest pain patients should receive an ECG, the atypical symptoms that might be present, and the baseline triage level recommended before other factors warrant its change.
- Increase exposure to a variety of patient presentations.
An organization might employ retrospective chart review as performed by a peer. This allows the original triage nurse to receive feedback on his/her evaluation while giving the evaluating nurse perspective on another patient encounter, thus improving their experience and exposure to a variety of cases. This increased exposure can better prepare the evaluating nurse for a similar future encounter.
- Evaluate common leveling mistakes.
To make the best rapid decision in the moment, many organizations find that a triage level of 3 is applied to an overwhelming number of patient encounters. Retrospective chart review systems allow nurse managers to review the breakdown of records based on triage level and evaluate whether these percentages are skewed. In the example report shown below, you can see that 30% of cases seen were given a Level 3. If this number seems abnormally high or low, it can be a signal to a nurse manager that there might be a knowledge gap worth addressing.
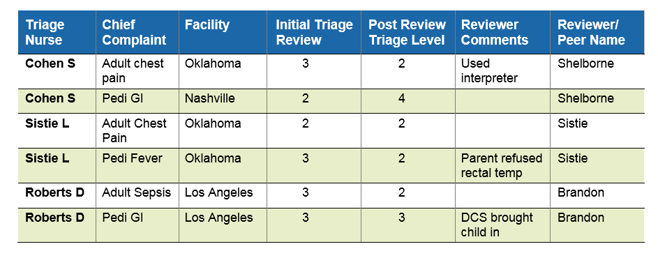
Similarly, a nurse manager might run a report including initial triage level and post review triage level to identify where an individual nurse might be struggling to grasp the intricacies of ESI or CTAS. With this information, performance improvement plans can be developed to address any shortcomings.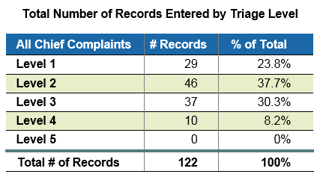
- Confirm Documentation Accuracy.
In the interest of both patient safety and loss prevention, a nurse manager is likely interested in whether the department is documenting to the extent recommended. Reporting can illuminate where nurses lack important documentation elements that could be critical in the accurate leveling of a patient.
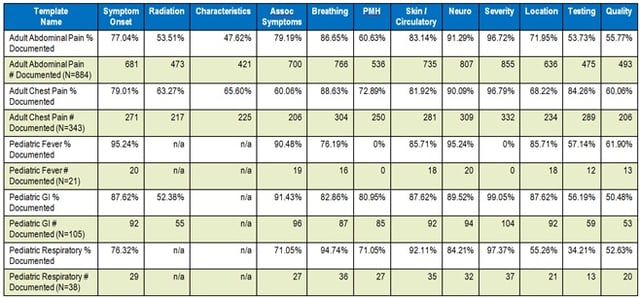
This sample report shows documentation completion stratified by chief complaint. In this example, you’ll see that in Adult Abdominal Pain patients, only 54% of charts include the radiation of pain element documented, but 86% of charts documented breathing status. This can be used to identify the most commonly missed items in chart documentation and target these areas for improvement with an education and observation plan.
While a triage competency validation process likely includes more than one method of measurement, the inclusion of retrospective chart review is one of the most critical components.
What tools do you use in your triage competency validation process? Do you agree with these benefits of chart review? Or do you have any disadvantages to report? We’d love to know. Email us to share your stories.
Learn more about TSG's retrospective self-assessment program here.
References:
1https://sjtrem.biomedcentral.com/articles/10.1186/s13049-015-0142-y


