Many organizations that study medical liability trends often point to breakdowns in communication, cognitive errors, lapse in clinical judgement, etc. as the main contributing factors that cause diagnosis-related claims. Because 60% of Emergency Medicine claims are diagnosis-related, every health care organization should have a strategy for mapping and organizing the most common clinical risk areas that physician’s face. Below we outline a tool that aims to help health systems organize a strategy to address the most frequent and severe malpractice claims.
 After completing this exercise, organizations should gain a clearer understanding about the areas of exposure and conditions that have historically led to litigation for their providers. It is also a good mapping tool to help tie the cost of those claims to the specific adverse events for the financial stakeholders. This exercise can also serve as a good analysis for leadership to populate in hopes of validating the efficacy of their existing risk mitigation solutions.
After completing this exercise, organizations should gain a clearer understanding about the areas of exposure and conditions that have historically led to litigation for their providers. It is also a good mapping tool to help tie the cost of those claims to the specific adverse events for the financial stakeholders. This exercise can also serve as a good analysis for leadership to populate in hopes of validating the efficacy of their existing risk mitigation solutions.
Completing the Risk Analysis
To analyze your risk mitigation strategy, we recommend you start with a basic, high level outline of exposure (below left), current risk mitigation programs in place to address that exposure (below middle), and the impact of those programs on outcomes (below right). 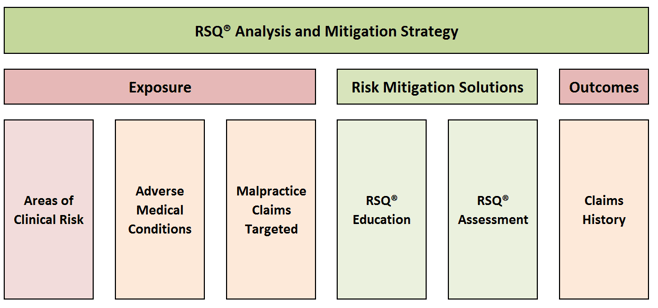
Step 1
Within the area of identifying exposure, we recommend categorizing specific Areas of Clinical Risk unique to each specialty. For example, in Emergency Medicine, we often start with areas of the body and common presenting Chief Complaints that could reasonably give rise to adverse events. The image below does not cover all Areas of Clinical Risk, but rather provides a very focused look at a few high-risk areas. Some organizations may want to pull their patient volume information for their Emergency Department to gain an even better understanding of the frequency of those high-risk presentations (like Head Injury).
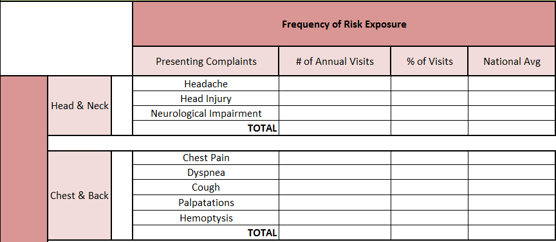
From those presenting complaints (Frequency of Risk Exposure), we then list which severe diagnosis-related malpractice claims are often associated with those presenting complaints. As an example, the image below only focuses on a few key areas (Head & Neck; Chest & Back).
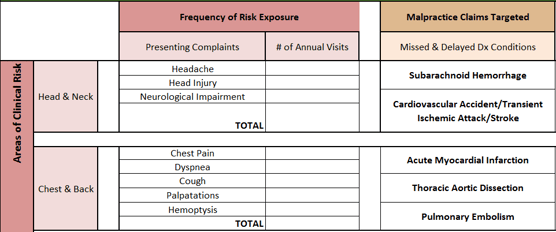
Step 2
The next step of this exercise is to place your current internal process in the blue column to map how your organization currently addresses mitigating this risk.

Step 3
The last step of building a profile and mapping clinical risks is contingent upon pulling your previous five years of loss runs for that specialty. In this example, we have focused on the most common chief complaints related to diagnosis-related claims.
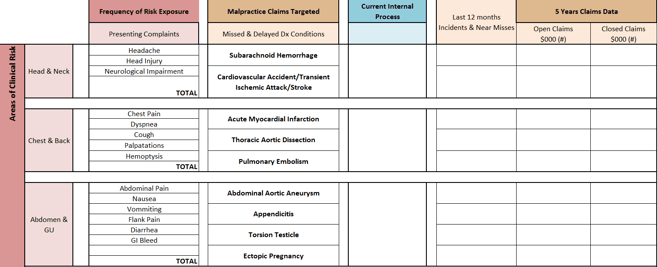
Because of the emphasis on diagnosis-related errors and litigation, we presume that many hospitals and health systems have existing processes in place to mitigate the risk against many of these claims. However, given the vast number of presenting complaints and complexities in Emergency Medicine, many organizations may not have their arms around the top 20 most common diagnosis-related claims that could surface at any point.
We recommend use of this tool to organize your strategy with loss prevention and patient safety in Emergency Medicine. To gain access to this worksheet, please email Brant Roth at broth@thesullivangroup.com.


