[9 MIN READ]
Updated: March 18, 2020
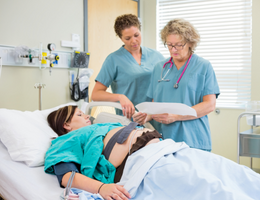
Working on the front lines of an obstetric unit is fraught with vulnerability and uncertainty during these early stages of the unprecedented COVID-19 pandemic. Your obstetric team has never before been so codependent in maintaining safety for you and your entire community. Arming yourself and teammates with the most current knowledge will help to keep you, your family, and your patients as safe as possible.
Since much is unknown about the novel coronavirus, review of daily updates and evolving information from our health experts is important. Staying knowledgeable and well-informed will require ongoing review of CDC updates and government notifications, as well as guidelines from our own health professionals like AWHONN and ACOG. All healthcare providers and frontline OB staff should work together to help ensure that everyone is practicing using the most current information. Teamwork along with shared learning will help everyone stay informed.
To keep yourself and your obstetric peers current on COVID-19, The Sullivan Group is providing this summary of recent information from the CDC and ACOG (last updated March 18, 2020).