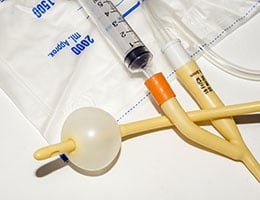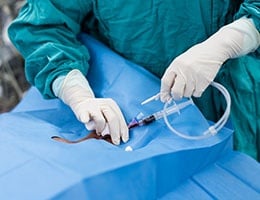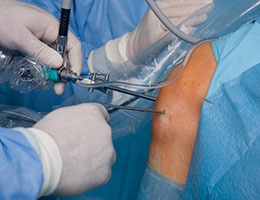
Surgical Site infections (SSIs) occur in 2% to 5% of surgery patients. This category of infection comprises approximately 22% of all healthcare-associated infections and has a 3% mortality. Patients with SSIs require significant care and average 7 to 10 days of increased length of hospital stay. The cost of providing care for a single SSI ranges from $3,000 to $29,000. The total cost of care for SSIs is estimated at $10 billion dollars per year. There are of course additional expenditures for outpatient care, readmissions, and care of long-term disabilities.